Why Modern Science is Rethinking the War on Saturated Fat?
The Diet Cholesterol Hypothesis is Broken For over six decades, the “Diet-Heart Hypothesis” has dominated public health messaging. This theory suggests that eating saturated fat raises blood cholesterol, which in

The Diet Cholesterol Hypothesis is Broken
For over six decades, the “Diet-Heart Hypothesis” has dominated public health messaging. This theory suggests that eating saturated fat raises blood cholesterol, which in turn causes heart disease. However, as we approach 2026, the scientific community is facing a significant flip-flop.
Modern data suggests that the fear of natural fats was not only premature, but may have actively contributed to today’s metabolic health crisis, including rising rates of obesity, diabetes, and cardiovascular dysfunction.
Challenging the Nutritional Status Quo
In her recent analysis for The Hill, investigative journalist Nina Teicholz points out a critical historical error that reshaped modern nutrition.
She notes that the U.S. Dietary Guidelines, first launched in 1980, were implemented without rigorous clinical trial evidence to support the demonization of saturated fat. At the time, even the National Academy of Sciences warned that the evidence linking saturated fat to heart disease was “inconclusive.”
Despite these warnings, dietary policy moved forward. Teicholz argues that by officially labeling animal fats as dangerous, the government initiated a massive, uncontrolled nutrition experiment on the American population.
As people were encouraged to replace butter, eggs, and red meat with highly processed vegetable oils and so-called “heart-healthy” grains, the unintended consequences became impossible to ignore:
- Obesity rates surged
- Type 2 diabetes skyrocketed
- Metabolic syndrome became the norm rather than the exception
Rather than improving heart health, low-fat dietary guidance may have accelerated chronic disease.
The Global Reality Check: The PURE Study
The most substantial reality check comes from the Prospective Urban Rural Epidemiology (PURE) study, one of the largest nutritional studies ever conducted.
This project followed 135,000 individuals across 18 countries, examining dietary patterns and long-term health outcomes. By studying global populations—not just Western, industrialized nations—researchers uncovered a striking trend:
- High carbohydrate intake (over 60% of daily calories) was associated with a 28% increased risk of death
- Higher fat intake was linked to a lower risk of stroke
- Saturated fat intake showed no significant increase in cardiovascular mortality
These findings challenged decades of nutritional dogma and suggested that refined carbohydrates, not natural fats, may be a primary driver of poor health outcomes.
Fat: More Than Just Calories
From a biological and evolutionary perspective, fat is not merely an energy source—it is a critical structural componentof human physiology.
Brain Composition
Your brain is approximately 60% fat. Saturated fats and cholesterol are essential for maintaining the integrity of cell membranes and the myelin sheath, which insulates nerves and allows fast, efficient signaling. Without adequate fat intake, neurological function may suffer.
Nutrient Absorption
Many essential micronutrients—specifically Vitamins A, D, E, and K—are fat-soluble. Without sufficient dietary fat, your body cannot efficiently absorb these nutrients, regardless of how many vegetables you consume.
Hormonal Satiety
Fats and proteins stimulate the release of satiety hormones such as cholecystokinin (CCK). These signals tell your brain that you are full, helping regulate appetite and preventing the insulin roller coaster caused by high-carbohydrate, low-fat processed foods.
Moving Forward with Metabolic Clarity
The so-called “Cholesterol Con” is steadily losing its grip as more physicians and researchers reassess the actual evidence. When we prioritize nutrient-dense, whole-food fats, we are not simply eating for taste—we are providing our bodies with the raw materials needed for neurological health, hormonal balance, and metabolic stability.
This holiday season, as you navigate the festive table, remember that the science is shifting. Prioritizing high-quality proteins and natural fats is not an indulgence—it is an evidence-based approach to long-term health.
Frequently Asked Questions (FAQ)
Is saturated fat actually bad for heart health?
Current evidence shows that saturated fat alone is not a reliable predictor of heart disease. Overall dietary patterns, inflammation, and refined carbohydrate intake play a larger role.
What replaced saturated fat in the modern diet?
Saturated fats were largely replaced with refined carbohydrates, sugar, and industrial seed oils—foods now strongly linked to metabolic disease.
Does dietary cholesterol raise blood cholesterol?
For most people, dietary cholesterol has minimal impact on blood cholesterol levels due to tight regulation by the liver.
Why was the low-fat message so influential?
Early observational studies and political pressure led to dietary guidelines that were never properly validated through long-term clinical trials.
What fats should be prioritized today?
Whole-food fats such as butter, olive oil, eggs, fatty fish, and unprocessed animal fats are increasingly supported by modern research.
Understanding Cholesterol: What It Is, What the Numbers Mean, and How It’s Tested
To understand why the Diet Cholesterol Hypothesis is broken, it’s essential to clarify what cholesterol actually is—and what modern medicine measures when it labels cholesterol as “good” or “bad.”
What Is Cholesterol?
Cholesterol is a wax-like, fat-based molecule that is essential for human life. Nearly every cell in your body uses cholesterol for critical functions, including:
- Building and maintaining cell membranes
- Producing hormones such as estrogen, testosterone, and cortisol
- Creating vitamin D
- Forming bile acids, which help digest fat
Importantly, about 75–80% of your cholesterol is produced by your liver, not consumed through food. Your body tightly regulates cholesterol production based on its needs, increasing or decreasing output as necessary.
Cholesterol itself is not inherently harmful—it is a vital biological building block.
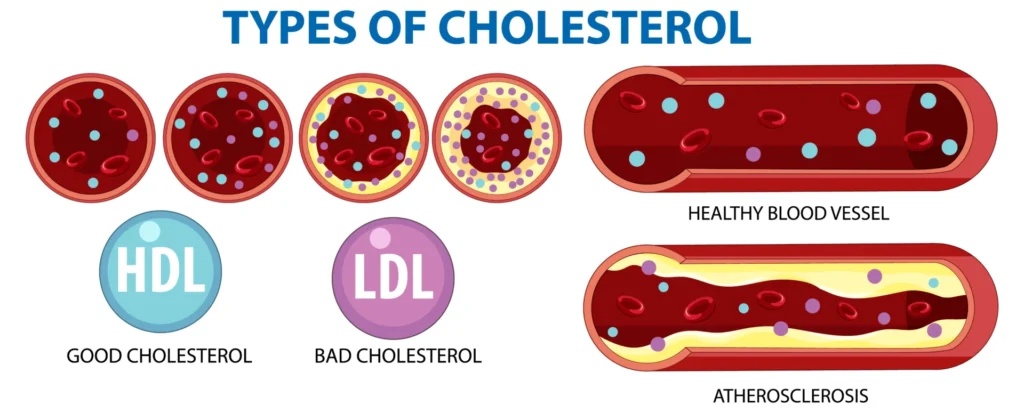
“Good” vs. “Bad” Cholesterol: A Simplified Story
Cholesterol does not travel freely in the bloodstream. Because fat and water don’t mix, cholesterol is transported by lipoproteins, which act like delivery vehicles.
LDL (Low-Density Lipoprotein) – Often Called “Bad” Cholesterol
LDL particles deliver cholesterol from the liver to tissues that need it. For decades, higher LDL numbers were assumed to directly cause heart disease.
However, modern research shows that:
- LDL is not inherently dangerous
- Risk depends on particle size, oxidation, inflammation, and insulin resistance
- Many people with elevated LDL have no cardiovascular disease
HDL (High-Density Lipoprotein) – Often Called “Good” Cholesterol
HDL helps transport excess cholesterol back to the liver for recycling or removal. Higher HDL levels are generally associated with better metabolic health, though simply raising HDL does not automatically reduce risk.
What Are Considered “Bad” Cholesterol Levels?
Traditional reference ranges (still commonly used) include:
- Total Cholesterol:
- Desirable: under 200 mg/dL
- LDL Cholesterol:
- Optimal: under 100 mg/dL
- Borderline high: 130–159 mg/dL
- HDL Cholesterol:
- Low (higher risk): under 40 mg/dL
- Protective: 60 mg/dL or higher
- Triglycerides:
- Normal: under 150 mg/dL
However, many clinicians now recognize that triglyceride-to-HDL ratio, insulin sensitivity, and inflammation markers are often more predictive of heart disease risk than LDL alone.
A person with:
- High LDL
- Low triglycerides
- High HDL
- Good metabolic health
may be at lower risk than someone with “normal” LDL but high blood sugar and chronic inflammation.
Written by Bryan Treacy for ravoke.com — and at Ravoke we proudly support women’s health. Dr. Bryan Treacy’s journey began with over three decades of dedicated service as an Obstetrician and Gynecologist. His extensive experience in women’s health laid a strong foundation in medical science and patient care. Recognizing the limitations of traditional medicine, Dr. Treacy transitioned to holistic health consultancy, merging scientific knowledge with a comprehensive understanding of wellness.








