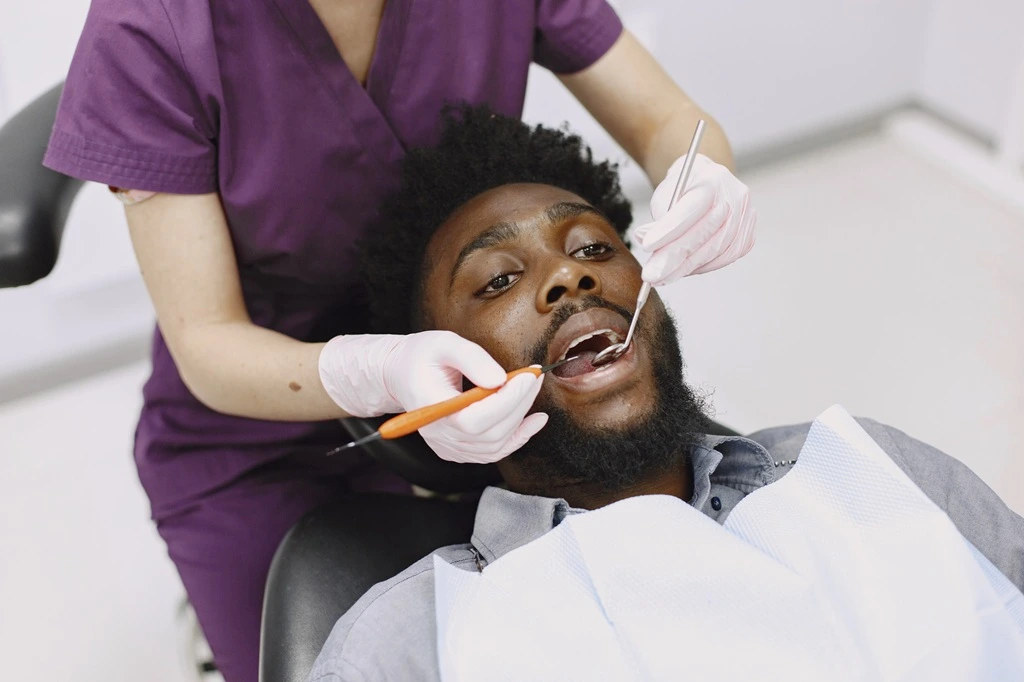
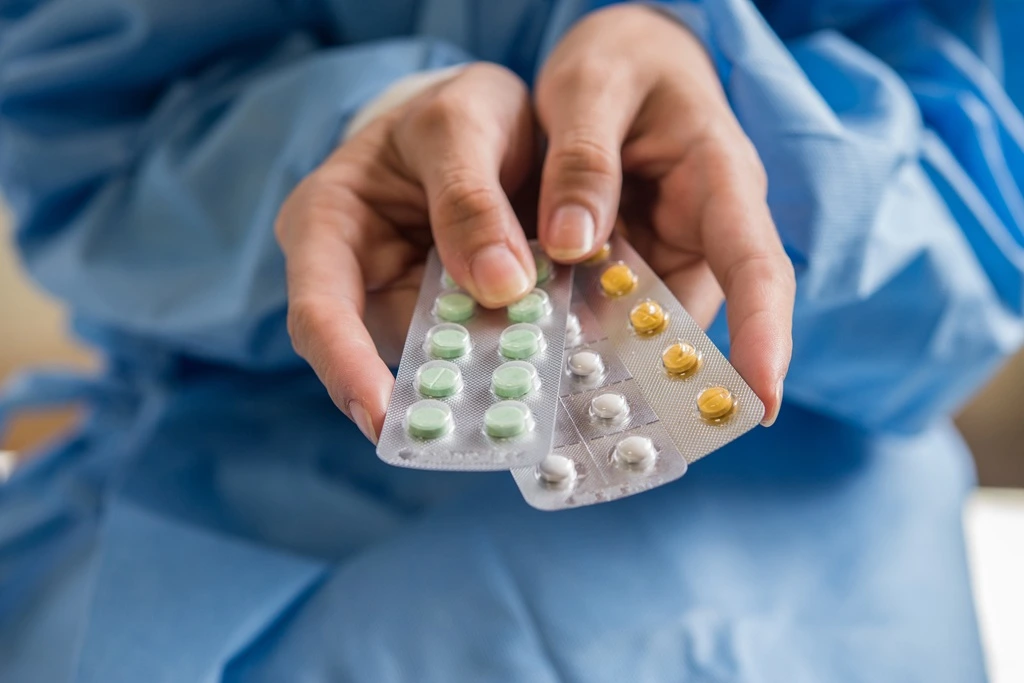
Smart Ways to Avoid Unneeded Antibiotics at the Dentist
By Gloria Lancer for Ravoke.com Why dental antibiotic use is under scrutiny Antibiotics are commonly prescribed in dental care, especially for procedures like tooth extractions or infections. But growing evidence
By Gloria Lancer for Ravoke.com
Why dental antibiotic use is under scrutiny
Antibiotics are commonly prescribed in dental care, especially for procedures like tooth extractions or infections. But growing evidence suggests that a large portion of these prescriptions may not be necessary—and could even pose risks to patients.
Data from the IQVIA Institute for Human Data Science shows that dentists issue tens of millions of antibiotic prescriptions each year in the United States. However, only a small percentage are used to treat active infections. Many are given as a precaution before or after procedures, even when the likelihood of infection is low.
Health experts warn that this pattern contributes to larger public health concerns, including Antimicrobial resistance—a growing problem that makes infections harder to treat over time.
Why unnecessary antibiotics can be harmful
Taking antibiotics when they aren’t needed doesn’t improve recovery—and it can lead to complications. These include allergic reactions, digestive issues, and infections caused by harmful bacteria like Clostridioides difficile infection, which can cause severe diarrhea and, in some cases, life-threatening illness.
The more frequently antibiotics are used, the less effective they become. Over time, bacteria adapt, making standard treatments less reliable for everyone.
Start with strong oral health habits
One of the most effective ways to avoid unnecessary antibiotics is to prevent dental problems in the first place.
Good oral hygiene—regular brushing, flossing, and routine dental visits—can significantly reduce the risk of infections. Addressing dental pain or swelling early often allows dentists to treat the issue directly, without relying on medication.
In many cases, procedures such as fillings, root canals, or extractions can resolve the problem without antibiotics if handled promptly.
Don’t assume antibiotics are always needed
Many people expect antibiotics when they experience dental pain or undergo procedures, but they are not always required.
Guidelines from the American Dental Association recommend antibiotics only in specific situations—such as when there are clear signs of a spreading infection or systemic symptoms like fever.
Similarly, the American Heart Association has narrowed its recommendations for preventive antibiotics. Today, they are advised only for patients with certain high-risk heart conditions, rather than broadly for anyone undergoing dental work.
Ask questions before accepting a prescription
If your dentist suggests an antibiotic, it’s reasonable—and encouraged—to ask why. Understanding whether the medication is essential can help you make informed decisions about your care.
You might ask:
- Is this antibiotic necessary for my condition?
- Are there alternative treatments?
- What happens if I wait and monitor symptoms?
In some cases, dentists may recommend delaying the prescription and only using it if symptoms worsen, such as developing a fever or increased swelling.
Be aware of side effects and risks
Not all antibiotics carry the same risks. Some, like Clindamycin, are more strongly associated with complications like C. difficile infections.
Before starting any antibiotic, ask about common side effects and warning signs of serious reactions. While mild stomach upset can occur, persistent diarrhea, severe abdominal pain, or dehydration may require immediate medical attention.
Share your full medical history
Your dentist may not have access to your complete health records, so it’s important to speak up about past reactions to medications.
For example, a history of severe antibiotic-related illness or digestive issues could influence which medications are appropriate. Providing accurate information helps reduce the risk of complications.
Rethink antibiotic allergies
Many people believe they are allergic to certain antibiotics—particularly penicillin—but research shows that true allergies are far less common than reported.
Mislabeling an allergy can lead to the use of alternative antibiotics that may be less effective or carry higher risks. If there’s uncertainty, consulting a specialist for testing can help clarify whether an allergy is real.
Shorter treatments may be enough
Traditional antibiotic courses often lasted a week or longer, but newer research suggests shorter durations can be just as effective in many cases.
The Centers for Disease Control and Prevention advises that minimizing exposure to antibiotics—while still treating infections effectively—can reduce the risk of side effects and resistance.
Patients should always follow their provider’s instructions but can ask whether a shorter course is appropriate.
Extending the conversation: changing habits in dental care
The issue of antibiotic overuse in dentistry reflects a broader shift in healthcare toward more cautious and evidence-based prescribing. For decades, antibiotics were often viewed as a low-risk safety net—something that could prevent complications even when the likelihood of infection was minimal. Today, that mindset is evolving.
One major driver of change is the growing awareness of antimicrobial resistance. As bacteria become more resistant to existing drugs, the medical community is under increasing pressure to preserve the effectiveness of current treatments. Dentistry plays a significant role in this effort, given the high volume of prescriptions written each year.
Another factor is patient expectation. Many individuals still associate antibiotics with faster recovery, even when they are not medically necessary. This can create pressure on dentists to prescribe them “just in case.” Educating patients about when antibiotics are—and are not—helpful is key to changing this dynamic.
Technology and research are also helping reshape best practices. Improved diagnostic tools and updated clinical guidelines are making it easier for providers to determine when antibiotics are truly needed. At the same time, ongoing studies continue to highlight the risks associated with unnecessary use, reinforcing the importance of restraint.
Ultimately, reducing inappropriate antibiotic use requires a shared effort. Dentists must follow evolving guidelines, and patients should feel empowered to ask questions and understand their treatment options. By working together, both providers and patients can help ensure antibiotics remain effective for those who genuinely need them.
Frequently Asked Questions (FAQ)
Why do dentists prescribe antibiotics?
Dentists may prescribe antibiotics to treat infections or, in some cases, to prevent them. However, preventive use is often unnecessary for most patients.
Are antibiotics always needed after dental procedures?
No, many procedures do not require antibiotics. Treatments like fillings or extractions often resolve the issue without medication.
What are the risks of taking antibiotics unnecessarily?
Risks include allergic reactions, digestive issues, and infections like C. difficile, as well as contributing to antibiotic resistance.
What is antimicrobial resistance?
It occurs when bacteria evolve to resist antibiotics, making infections harder to treat and increasing the risk of complications.
Should I question my dentist about antibiotics?
Yes, it’s appropriate to ask whether an antibiotic is necessary and if there are alternative options.
Are shorter antibiotic courses effective?
In many cases, yes. Shorter courses can treat infections effectively while reducing the risk of side effects.
References
- IQVIA Institute for Human Data Science – Data on dental antibiotic prescribing trends in the United States.
- American Dental Association – Guidelines on antibiotic use in dental care.
- American Heart Association – Recommendations for preventive antibiotics in dental procedures.
- Centers for Disease Control and Prevention – Antibiotic stewardship and resistance prevention guidance.
- Research studies on antibiotic prescribing practices and resistance published in peer-reviewed medical journals.